|
New research demonstrates antiparasitic drug turns lethal for malaria-carrying mosquitoes showing promising future for the drug. Preliminary analysis showed that the drug reduced malaria cases in children under 5 by 16%. The trends are encouraging for the drug and it might become part of national malaria control programs.
Ivermectin a well known antiparasitic drug for treatment of a wide range of parasite infestations from head lice, scabies, river blindness (onchocerciasis), strongyloidiasis, trichuriasis, and lymphatic filariasis, may have another hidden benefit.
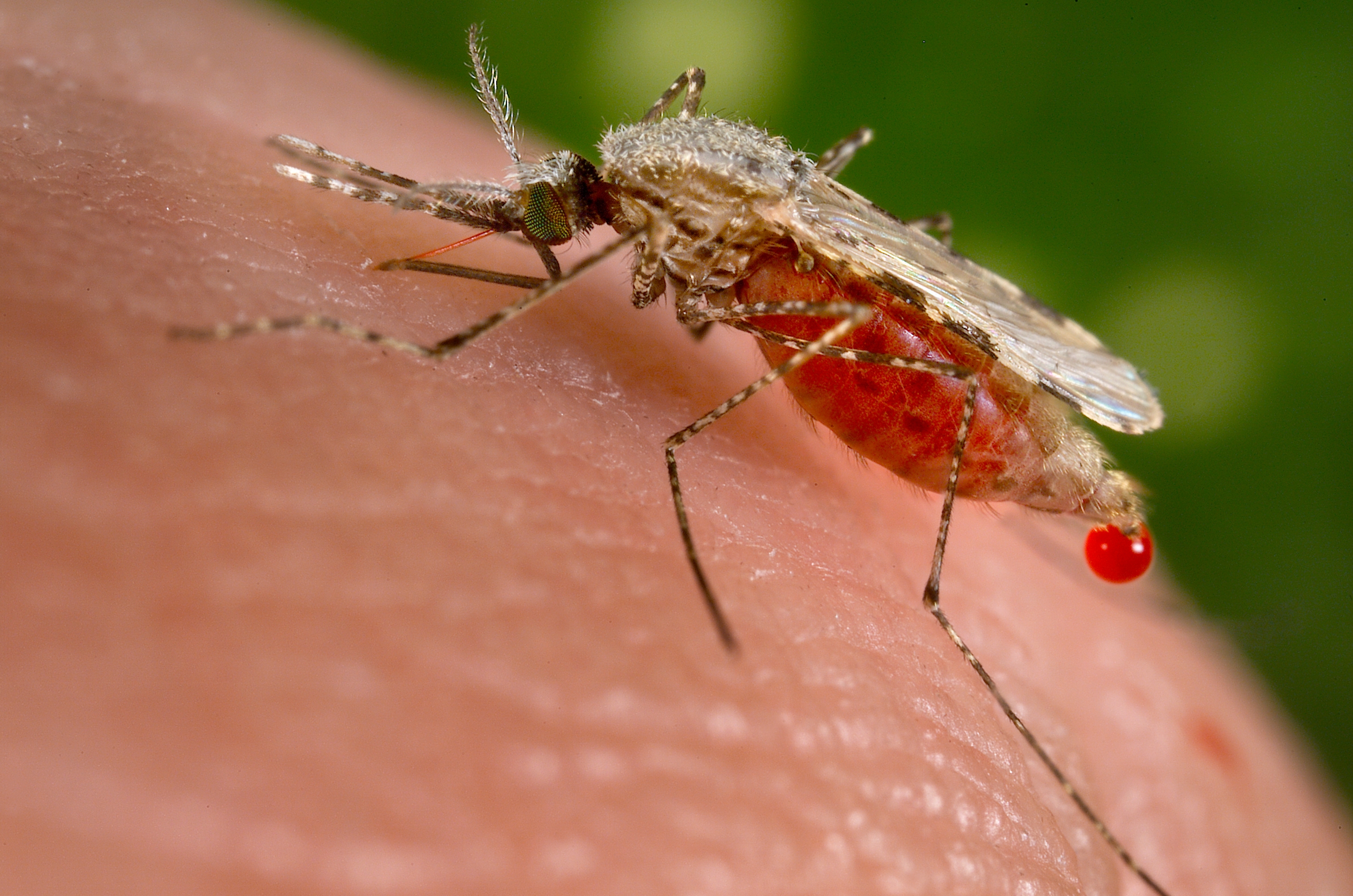
Mosquitoes of the genus Anopheles and only females of the species are capable of transmitting the malaria pathogen a protozoa, of genus Plasmodium, which undergoes a series of infection steps before arriving at the mosquito’s salivary gland, from where it ultimately gets transmitted to the human host during blood meal. Malaria has been a well known killer in the tropical regions of the globe killing more peoples combined who died from outer causes. The data for malaria infection and transmission is staggering as each year, the disease infects more than 200 million people, causing 429,000 deaths — and the situation seems to get worse as despite spending billions on malaria eradication programs, we seem to have reached a plateau. Meanwhile mosquitoes are becoming increasingly resistant to insecticides, which is forcing researchers to think of all sorts of new solutions like a malaria vaccine, genetically engineering mosquitoes so they wipe themselves out and many more. Previous studies have found that malaria-carrying mosquitoes would die after sucking the blood from individuals who had taken ivermectin, researchers have known for decades that the drug also kills insects if they ingest it. Brian Foy, a medical entomologist at Colorado State University, Fort Collins, believes that makes it a prime candidate in the fight against malaria. If enough people in an area have ivermectin in their blood, says Foy, some of the female mosquitoes that bite them will die, whereas others will be too weakened to pass on the malaria parasite. Foy has shown in lab studies that the approach holds promise, and co-founded a research network last year to study the concept further, to show that ivermectin actually has an impact on malaria in the field, Foy teamed up with Roch Dabiré, a researcher at the Institute of Health Studies in Bobo-Dioulasso, Burkina Faso. The scientists went to eight villages near the town of Diébougou, in the southwest of the country. At the start of the trial, in July, the population of all villages received one dose of ivermectin and another drug, albendazole; this standard combination is given twice yearly around Burkina Faso to control elephantiasis and soil-transmitted worms. In four of the villages, this was followed by ivermectin tablets every 3 weeks for the entire population except pregnant women and children under 90 centimeters tall, who may be at higher risk of side effects. The four other villages served as controls; they received no drugs after the first dose. The trial is still ongoing and will conclude in November. But an interim analysis presented today by Foy and Dabiré at the annual meeting of the American Society of Tropical Medicine and Hygiene suggests that the drug is already having an impact. Among children under the age of 5—the group at the highest risk of severe disease and death from malaria—there were 16% fewer cases in the villages that received ivermectin at 3-week intervals. That translates to 94 cases averted so far this season in the four villages. The full results will take some time to analyze, and the study will need to be repeated at a larger scale to see if the findings hold up, Dabiré says. If they do, ivermectin could be another weapon in the antimalaria arsenal, Foy says. He adds that it wouldn’t replace other measures, such as insecticide-treated bed nets. It’s an interesting approach that should be explored further, says Michel Boussinesq, who studies ivermectin at the Institute of Research for Development in Montpellier, France. But the need to give ivermectin every 3 weeks could be a logistical problem, he says. Boussinesq and his colleagues are working on an ivermectin implant for animals that instead releases the drug slowly and offers long-term protection. Such implants aren’t likely to be acceptable for use in humans, Foy says—but he points out that ivermectin would only be given during the rainy season, when malaria mosquitoes are active. The season lasts about 6 months in the region where the study took place and even less than that farther north, in the Sahel region. “I think that’s feasible,” Foy says. Willem Takken, a medical entomologist at Wageningen University and Research Centre in the Netherlands, sees another, fundamental problem: Mosquitoes have developed resistance against almost any chemical that humans have thrown at them. He says that’s bound to happen with ivermectin, too. That’s why, despite the encouraging data, “I find it hard to get enthusiastic about this,” Takken says. He believes that nonchemical approaches, such as mosquito traps or bacteria that render mosquitoes unable to transmit pathogens, hold more long-term promise. ************************************************************ References:
1 Comment
|
AuthorHello! My name is Arunabha Banerjee, and I am the mind behind Biologiks. Leaning new things and teaching biology are my hobbies and passion, it is a continuous journey, and I welcome you all to join with me Archives
July 2022
Categories
All
|

 RSS Feed
RSS Feed



